Presidium Health • Patient Experience
The People’s Voice: What IEHP Members Tell Us About Presidium Health CalAim Program
We asked current Presidium Health members about their experience, what support helps most, and where the health system creates friction. The results validate a relationship-based, high-touch model designed for complex needs—delivered where the patient is.
Email survey (n=21) High-touch Enhanced Care Management Social + behavioral + navigation support
76%Rated overall experience Very Good
91%Feel Very Comfortable with the care team
92%Expressed praise or requested no changes

What this means
The strongest signal is trust: members report high satisfaction and comfort with the care team. The most helpful supports are consistently the drivers of avoidable utilization—food insecurity, behavioral health stressors, and health system navigation (benefits, care plans, and appointments).
Key takeaways
- Trust is a differentiator—members feel comfortable reaching out and relying on the team.
- High-touch is required—most members need monthly or more frequent support, and many need weekly engagement.
- Value concentrates in SDOH + navigation + behavioral support (food, stress/mood, benefits and care-plan understanding).
- Friction is still system-driven—insurance complexity, confusion about who to call, stress/overwhelm, and transportation barriers.
How Presidium responds
Presidium Health is built for complex members: a direct-to-patient, relationship-based model that reduces system friction by making support accessible, responsive, and practical—especially when needs are social, behavioral, and logistical.
Human-first communication Members most often prefer phone-first support, with texting as a strong secondary option.
Navigation that actually works We help members understand benefits, coordinate appointments, and reduce confusion about “what to do next.”
Addressing real drivers of utilization Food support, behavioral health stress, and housing instability are prioritized because they drive outcomes.
High-frequency engagement Our model is designed for continuous support—monthly, weekly, and during episodic crises.
“I finally had someone I could call who would actually help me figure things out.”Representative member feedback theme (relationship + navigation support)
Survey results (visual summary)
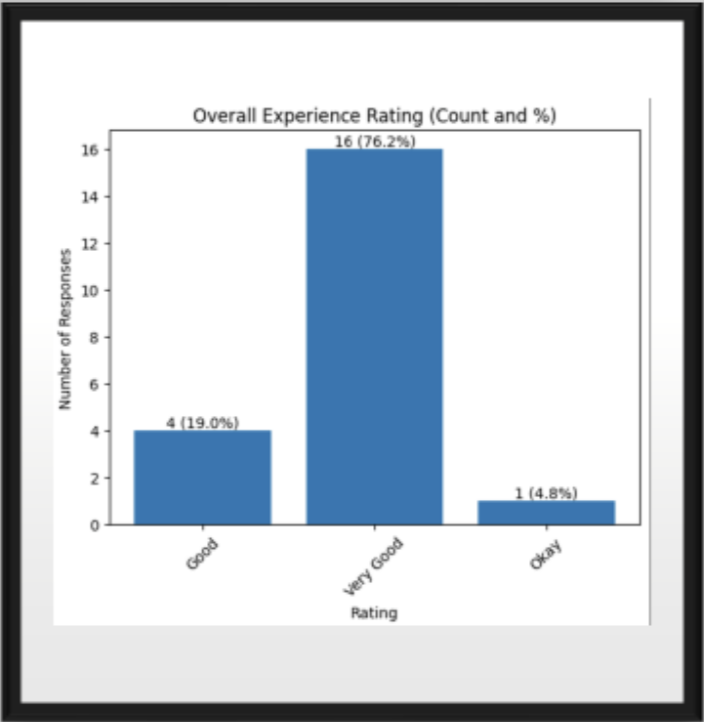
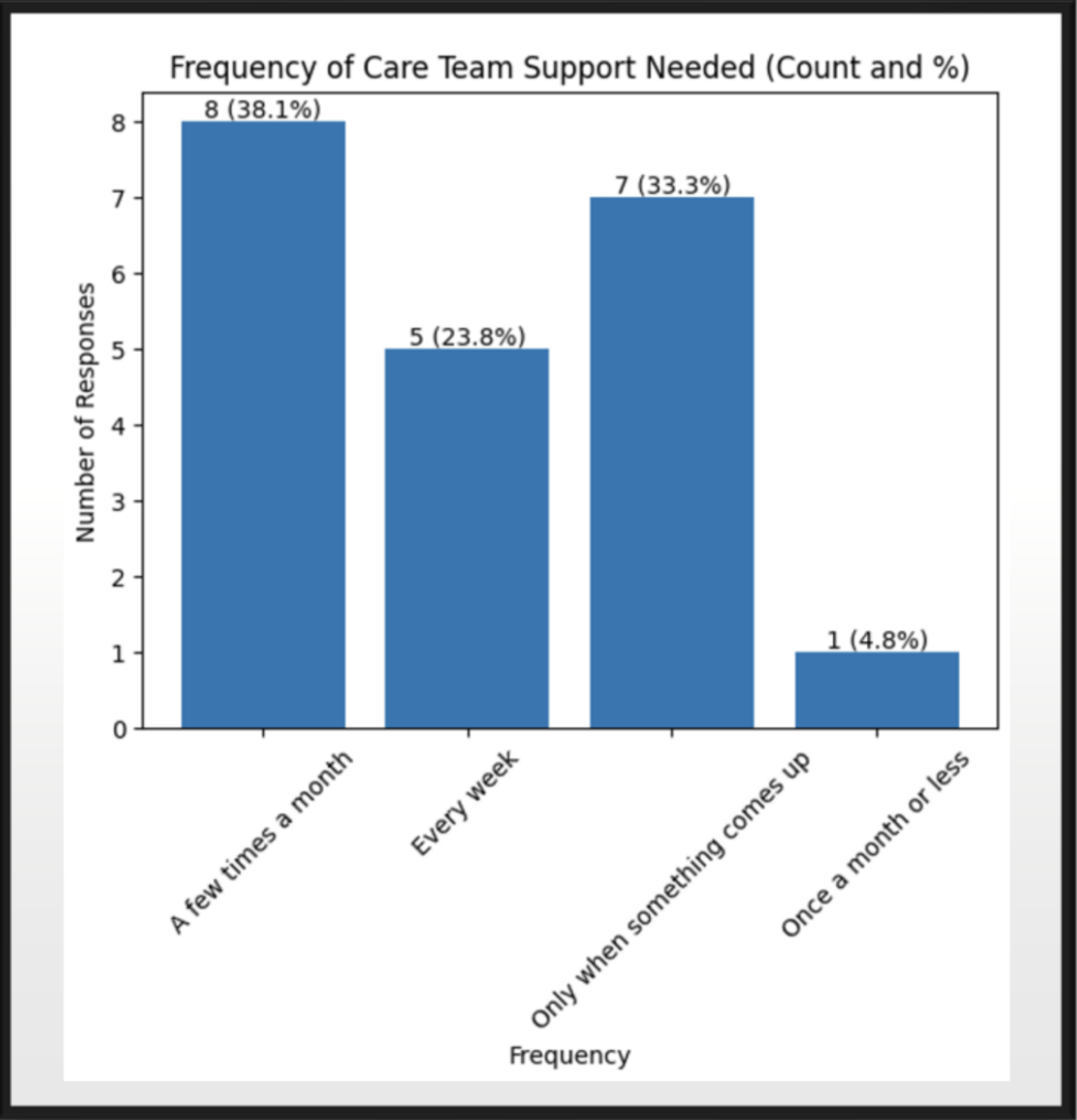
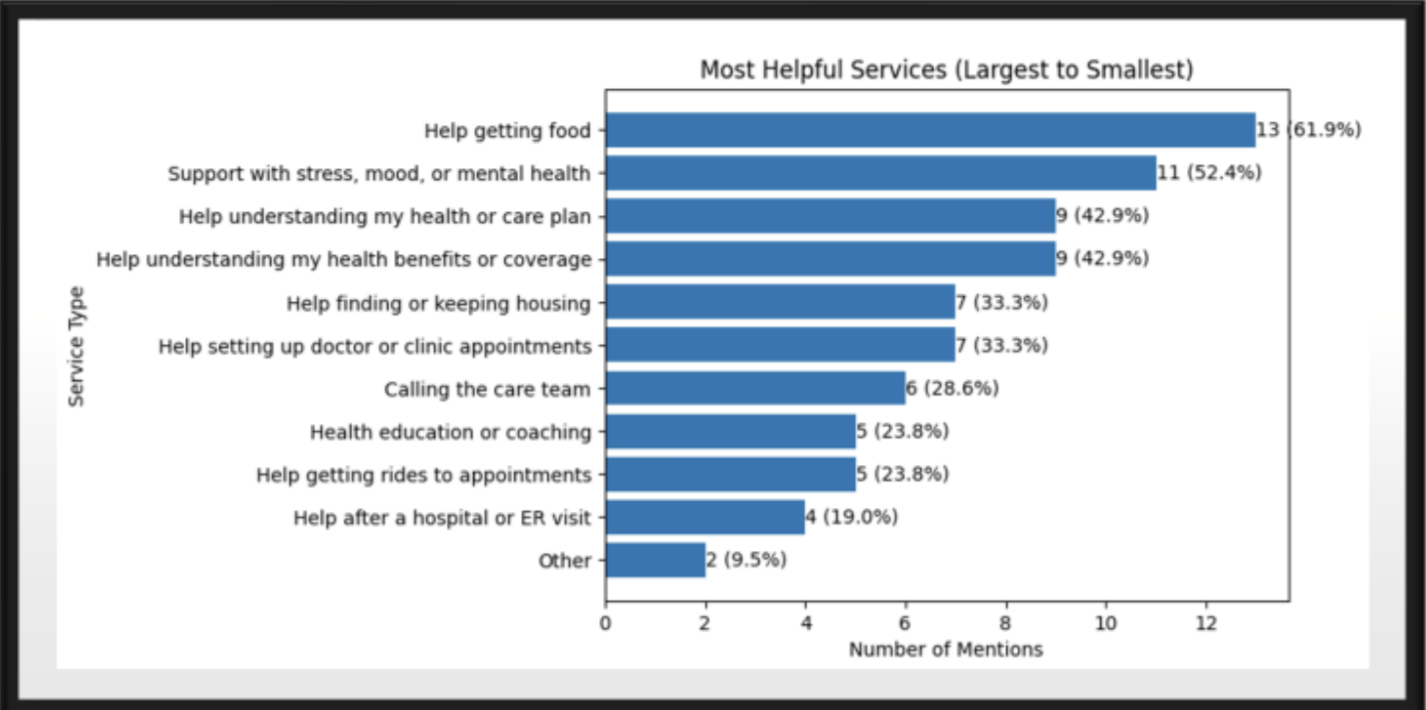

Interpretation: Why this matters for high-risk members
High-utilizer members often face a combination of medical complexity and social instability. The survey indicates that what members value most is not a single clinical intervention—it is the ability to reliably access help, reduce confusion, and resolve urgent needs before they escalate into avoidable emergency utilization.
Where Presidium creates leverage
- Food support and resource connection to reduce instability that worsens medical conditions.
- Behavioral health support to address stress, mood, overwhelm, and downstream adherence issues.
- Benefits + care-plan navigation so members understand coverage, next steps, and who to call.
- Appointment + transportation coordination to convert care plans into completed care.
- Relationship and trust so members reach out early—before crises become avoidable ED visits.
CalAIM Alignment: ECM & Community Supports with IEHP
Presidium Health partners with Inland Empire Health Plan (IEHP) to deliver services under California’s CalAIM (California Advancing and Innovating Medi-Cal) initiative, including both Enhanced Care Management (ECM) and Community Supports (CS).
How Presidium fits within CalAIM
- Enhanced Care Management (ECM): Comprehensive care coordination for high-risk, high-utilizer members
- Community Supports (CS): Services addressing social drivers of health such as food, housing, and recovery support
- Direct-to-patient delivery: Support delivered where the patient is—home, community, or non-traditional settings
Beyond minimum service expectations
While CalAIM reimbursement is often structured around defined service events (including one-time service fees for certain activities), high-risk members do not operate on a fixed schedule. Their needs fluctuate, and crises do not follow billing cycles. Presidium Health provides support as needed beyond the anticipated minimums within the CalAIM program to ensure our outcome-based ethos: stabilizing members, reducing avoidable utilization, and strengthening durable engagement.
Minimum vs. Outcome-Based Support

Structured program expectations
Many care models focus on discrete, time-bound interactions—often optimized around required checkboxes and service events.
Discrete touchpointsEvent-based tasksMinimum thresholds
Presidium’s outcome-based ethos
We maintain continuity and engage as needed—monthly, weekly, or during crises—so members are stabilized and supported in real time.
Monthly+ engagementWeekly support when neededCrisis responseContinuity & trust
CalAIM provides the framework. Presidium Health provides the execution.We align to program structure while delivering the high-touch reality complex members require.
Outcome-based care delivery We do not limit support to discrete billable events when a member needs stabilization, navigation, or crisis prevention.
High-touch engagement is validated by survey results Members report frequent needs—monthly or more often, with many requiring weekly contact or episodic crisis support.
Community Supports in real life Food, housing, transportation, and resource connection show up as top drivers of member-reported value.
Aligned with CalAIM objectives Reduced avoidable ED utilization, improved engagement, and addressing social drivers of health are central to our model.
Why this matters for plans and providers
- Stabilize high-utilizer members in the community
- Improve care plan adherence and follow-through
- Reduce avoidable emergency and inpatient utilization
- Address social and behavioral drivers of cost
- Create durable engagement with historically hard-to-reach populations
Want to learn more or refer a member?
Presidium Health provides enhanced, high-touch support for complex members—medical, behavioral, and social needs—through a direct-to-patient model. If you are a plan, provider, or member seeking support, contact us below.
Email: ASH@PRESIDIUMHEALTH.COM FOR CONTRACTING
Email: MELODY@PRESIDIUMHEALTH.COM FOR OPERATIONS AND SERVICES
Language access: English • Español • Farsi
Survey note: Summary based on an email survey of current Presidium Health members (n=21). Results reflect member-reported experience and priorities.
